A groin injury in hockey can become chronic and difficult to heal. A physiotherapist can assess it and develop a personalized treatment plan to help you return to play.
Throughout a season, groin injuries are more common in hockey than in other sports (1, 2). They can account for up to 10% of all hockey injuries and may cause difficulties with skating (1).
Groin injuries can occur up to five times more frequently at the start of the season (2). They are most common in athletes with insufficient strength in the hip adductors and abductors (1, 3).

What Is a Groin Injury?
Muscle injury to the hip adductors
A groin injury often involves the hip adductor muscles, which attach in this region (5). These inner-thigh muscles bring the leg toward the body and help control leg spacing. The adductor longus is the muscle most frequently affected (5).
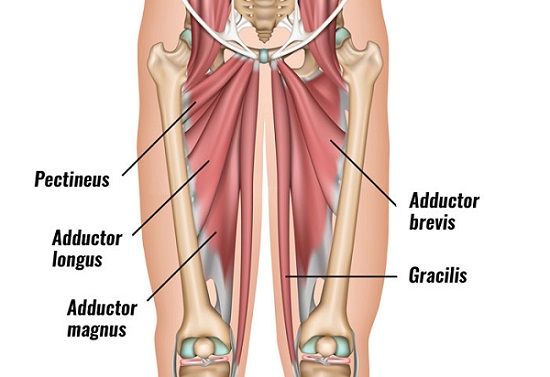
During a skating push-off, the hip adductors can be injured if overstretched. They can also contract improperly to stabilize the leg during push-off or to bring the leg back toward the body (recovery phase; 1, 3).
These injuries are classified into different grades based on signs and symptoms, as well as the recovery time required before returning to play (4, 5, 6).
| Grade | Signs and Symptoms | Recovery / Return to Play |
|---|---|---|
| 1 (mild) | Muscle stretch with pain but no weakness | 1–2 weeks |
| 2 (moderate) | Partial tear with pain, weakness, possible swelling and bruising | 4–6 weeks |
| 3 (severe) | Complete tear with pain, muscle retraction, significant weakness, bruising, possible swelling | 6–10 weeks |
Hip adductor muscle injury can be identified through a physiotherapy clinical assessment (3). For more severe injuries, MRI can evaluate the extent of the damage (3).
Femoroacetabular Impingement (FAI)
Hockey players, especially goalies, have a higher rate of hip joint injuries compared to other athletes (2, 3).
In femoroacetabular impingement, the hip joint no longer functions optimally. The femoral head no longer fits perfectly into the pelvis socket (called the acetabulum; 2, 3, 7).
Certain bony shape changes—known as “cam” or “pincer”—may develop. These changes cause abnormal friction in the joint, which can eventually damage a small structure crucial for hip stability: the labrum (2, 3, 7).
FAI, usually more chronic, may cause (3, 7):
- C-shaped groin pain
- Reduced hip mobility (flexion and internal rotation)
- Muscle weakness
- Difficulty performing squats, lunges, and skating
To detect anatomical hip changes, X-rays are usually performed (2). MRI can then assess whether non-bony structures, like the acetabular labrum, are affected (2).
How to Recover from a Groin Injury?
Muscle Injury to Hip Adductors
Acute Phase (1–7 days)
- Avoid movements or activities that cause pain in the short term (2).
- Gradually resume activities if pain-free (2).
- Avoid stretching during the first weeks following a strain (8).
- Restore hip internal rotation mobility (5).

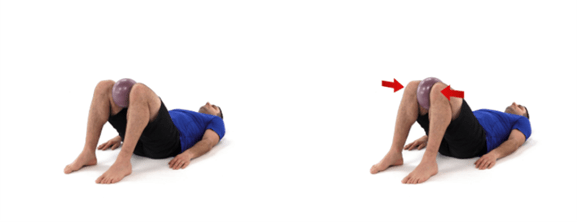
- Perform isometric (static) adductor strengthening exercises, such as squeezing a ball between the thighs and side planks (3, 6).

Subacute Phase (1–4 weeks)
- Once healing has progressed, gentle stretching can improve groin flexibility (8).
- Perform dynamic strengthening exercises, like lateral lunges and elastic band hip adductions.


Return-to-Play Phase (4 weeks–6 months)
- To improve muscle strength and prevent injuries: perform Copenhagen-style hip adductor exercises (6).

- Perform plyometric exercises (lateral and forward jumps, jump lunges, sprints).

Femoroacetabular Impingement
For FAI, it is very important to adapt activities to avoid pain (3). Physiotherapy is usually the primary approach. Hip mobility is gradually restored, and hip muscles are strengthened through various exercises (3). Return to sport is then gradual.
Some individuals with FAI experience persistent limitations in sports and daily activities. In these cases, surgery may be necessary (2). Return to sport after surgery typically takes three to four months (7).
How to prevent a groin injury
The risk of hip adductor injuries decreases when these muscles are at least 80% as strong as the hip abductors (1, 2). Therefore, regular adductor strengthening—often neglected at the gym—is important. Exercises mentioned in the subacute and return-to-play phases are excellent options to strengthen these muscles.
A proper warm-up before hockey is also essential. Warm-ups should include dynamic stretches and hockey-specific movements, such as squats and lunges (7).
Conclusion
For a groin injury that does not improve within a week despite avoiding painful activities, it is recommended to consult a healthcare professional. A physiotherapist can assess the injury and create a personalized treatment plan to safely resume your activities.
References
Rodriguez, R. (2020). Measuring the hip adductor to abductor strength ratio in ice hockey and soccer players: A critically appraised topic. Journal of Sport Rehabilitation, 29(1), 116-121.
Mosenthal, W., Kim, M., Holzshu, R., Hanypsiak, B., & Athiviraham, A. (2017). Common ice hockey injuries and treatment: a current concepts review. Current sports medicine reports, 16(5), 357-362.
Kuhn, A. W., Noonan, B. C., Kelly, B. T., Larson, C. M., & Bedi, A. (2016). The hip in ice hockey: a current concepts review. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 32(9), 1928-1938.
Chan, O., Del Buono, A., Best, T. M., & Maffulli, N. (2012). Acute muscle strain injuries: a proposed new classification system. Knee Surgery, Sports Traumatology, Arthroscopy, 20(11), 2356-2362.
Farrell, S. G., Hatem, M., & Bharam, S. (2023). Acute adductor muscle injury: a systematic review on diagnostic imaging, treatment, and prevention. The American Journal of Sports Medicine, 51(13), 3591-3603.
Thorborg, K. (2023). Current clinical concepts: Exercise and load management of adductor strains, Adductor ruptures, and long-standing adductor-related Groin Pain. Journal of athletic training, 58(7-8), 589-601.
LaPrade, R. F., Surowiec, R. K., Sochanska, A. N., Hentkowski, B. S., Martin, B. M., Engebretsen, L., & Wijdicks, C. A. (2014). Epidemiology, identification, treatment and return to play of musculoskeletal-based ice hockey injuries. British journal of sports medicine, 48(1), 4-10.
Physiopedia. Groin strain. Physiopedia. www.physio-pedia.com/Groin_Strain

