Conception difficulties, endometriosis, and assisted reproductive technology (ART) journeys can be physically and emotionally demanding experiences. Increasingly, women and couples are turning to osteopathy to help relieve pain, improve comfort, optimize pelvic health, and better cope with medical treatments.
Osteopathy does not replace reproductive medicine. Rather, it is part of a complementary approach focused on mobility, circulation, breathing, and stress regulation—factors that directly influence well-being and sometimes fertility.
Osteopathy and Fertility: What Can We Reasonably Expect?
According to several scientific sources, osteopathy may help women who are planning a pregnancy by working on:
- pelvic mobility
- pelvic vascularization
- lumbar and thoracic tension
- breathing
- stress
- the quality of the menstrual cycle
These factors do not “create” a pregnancy, but they may help to:
- improve comfort
- reduce certain types of pain
- support cycle regularity
- optimize the pelvic environment
- reduce tension or stress factors that may influence fertility

Osteopathy and Endometriosis: Relieving, Releasing, Supporting
Endometriosis affects approximately 1 in 10 women of reproductive age. It is often associated with pelvic pain, very painful periods, digestive issues, lower back pain, and sometimes fertility difficulties.
Osteopathy does not treat endometriosis itself, as it is a complex inflammatory condition. However, it may help reduce tension in the pelvis (small pelvis), improve the mobility of surrounding tissues, decrease menstrual pain, relieve lower back and abdominal pain, improve breathing and posture, and reduce fatigue related to pain.
Visceral, tissue-based, myofascial, and biodynamic techniques are particularly helpful for improving quality of life and reducing the impact of pain.
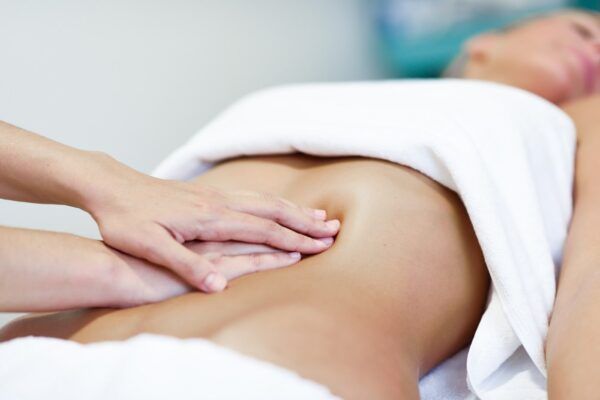
Osteopathy and Assisted Reproductive Technology (ART): Supporting the Body and the Experience
ART journeys (ovarian stimulation, insemination, IVF) can be demanding and often involve:
- hormonal treatments
- repeated medical examinations
- emotional stress
- fatigue
- pelvic or lower back tension
Several sources suggest that osteopathy may help to:
- improve pelvic mobility
- optimize blood and lymphatic circulation
- reduce menstrual or pelvic pain
- lower stress
- prepare the body to receive hormonal treatments
A recent survey conducted among patients undergoing medically assisted reproduction shows that the use of osteopathy is common and perceived as helpful support within a multidisciplinary approach.
Professional training programs for osteopaths also emphasize the importance of comprehensive, thoughtful care coordinated with medical teams.

Conclusion: Supporting the Body, Acknowledging the Experience, Creating Space
In fertility care, osteopathy can be a useful and effective complement to medical follow-up. It offers a space for regulation and well-being, which is essential in journeys that are often long and exhausting.
By working on:
- Tissue mobility: Tension in the pelvis, diaphragm, lower back, or fascia can influence circulation and comfort.
- Blood and lymphatic circulation: Better mobility promotes improved blood flow to the reproductive organs.
- The nervous system and stress: Gentle techniques help reduce nervous system hyperactivity, which is often heightened during ART treatments.
- Breathing and posture: The diaphragm plays a key role in pelvic circulation and stress management.
Osteopathy can play a valuable role in managing pain related to endometriosis, menstrual cycle disorders, fertility challenges, and assisted reproductive technology (ART) journeys.
It helps release tension, improve circulation, reduce pain, lower stress, and support the body at a time when it is under significant demand.
It is a gentle, human, holistic approach that deeply respects the journey of each woman and each couple.
Bibliography
De Strooper, L., Van Dun, P., & Van den Berg, F. (2024). Osteopathic manual treatment in women with endometriosis: A scoping review on clinical symptoms, fertility and quality of life. International Journal of Osteopathic Medicine, 52, 1–12. https://doi.org/10.1016/j.ijosm.2023.10.004
Schneider-Milo, A. (2011). The effectiveness of osteopathic treatment in women with endometriosis-related pain (Master’s thesis). Donau Universität Krems, Austria.
Waugh, E. (2019). Women’s experiences of osteopathic care whilst living with endometriosis (Master’s thesis). Unitec Institute of Technology, New Zealand.
Hensel, K. L., Buchanan, S., Brown, S. K., Rodriguez, M., & Cruser, D. A. (2019). OSTEOPATHIC MANIPULATIVE TREATMENT AND PAIN: Systematic review of randomized controlled trials. Journal of the American Osteopathic Association, 119(9), 559–573. https://doi.org/10.7556/jaoa.2019.091
Licciardone, J. C., Gatchel, R. J., & Aryal, S. (2016). Recovery from chronic low back pain after osteopathic manipulative treatment: A randomized controlled trial. Journal of the American Osteopathic Association, 116(3), 144–155. https://doi.org/10.7556/jaoa.2016.032
D’Alessandro, G., Cerritelli, F., & Cortelli, P. (2016). Sensitization and interoception as key neurological concepts in osteopathy and other manual medicines. Frontiers in Neuroscience, 10, 100. https://doi.org/10.3389/fnins.2016.00100
Cerritelli, F., et al. (2020). The effects of manual therapies on the autonomic nervous system: A systematic review. Frontiers in Neuroscience, 14, 600. https://doi.org/10.3389/fnins.2020.00600
Gameiro, S., Boivin, J., & Domar, A. (2013). Optimal psychological support for patients undergoing fertility treatment. Fertility and Sterility, 100(3), 731–737. https://doi.org/10.1016/j.fertnstert.2013.06.041
Pedro, J., et al. (2018). Psychological and emotional impact of infertility and ART: A systematic review. Reproductive Biomedicine Online, 36(6), 681–695. https://doi.org/10.1016/j.rbmo.2018.03.020
Schleip, R., & Müller, D. G. (2013). Training principles for fascial connective tissues: Scientific foundation and suggested practical applications. Journal of Bodywork and Movement Therapies, 17(1), 103–115. https://doi.org/10.1016/j.jbmt.2012.06.007
Bordoni, B., & Marelli, F. (2017). The fascial system and exercise intolerance in chronic diseases. Cureus, 9(7), e1418. https://doi.org/10.7759/cureus.1418

